We recently reached out to Dr. Antonios Gasparis, professor of surgery at Stony Brook University Hospital in New York, to learn more about his hospital’s venous thromboembolism (VTE) team. Upon its formation, the team was tasked with managing patients who have received IVC filters, including tracking eligible patients for outpatient follow-up and filter retrieval. Following is Dr. Gasparis’ description of the roles of the VTE team, results of protocol implementation, and suggestions for physicians who would like to create a similar program at their facility. Below, Dr. Gasparis answers the following question.
What are your current IVC filter retrieval protocols both with patients already under your care and when referred to you from another physician? Also, what are the key elements to success or overcoming challenges you experience within those protocols?
In 2009, we developed a VTE team at Stony Brook that includes a vascular surgeon champion and a dedicated nurse practitioner. It has since grown to include a second nurse practitioner and a phlebology fellow. The responsibilities of the VTE team include evaluation of patients not on any VTE prophylaxis, evaluation of all VTE events, managing patients on high-risk anticoagulants (Argatroban), identifying patients who are candidates for thrombolysis, management of patients receiving an IVC filter and outpatient follow-up.
With respect to patients who have an IVC filter placed at Stony Brook, they are entered into a custom database, and each patient is provided education about IVC filters. Significant attention is placed on the importance of retrieval prior to placement of the filter and at discharge.
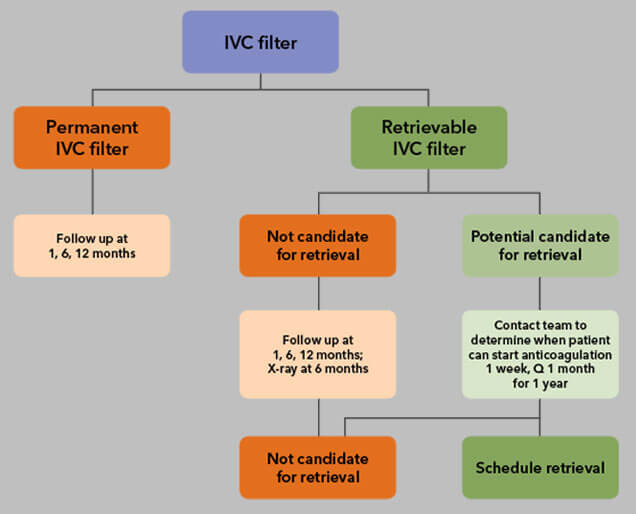
While in the hospital, each patient is monitored daily for the commencement of anticoagulation at therapeutic doses. When therapeutic, the primary team is contacted for feasibility of IVC filter retrieval while still an inpatient, and retrieval is then performed by vascular surgery. If a patient is discharged, the VTE team monitors the progress of patients by communicating with the physician monitoring the patient’s anticoagulation. When it is determined the patient can safely be anticoagulated, the patient is scheduled for a follow-up with the vascular surgery outpatient office and subsequently scheduled for IVCF retrieval, if appropriate. If the patient is not a candidate for retrieval, the VTE team performs a phone call follow-up at 6 months and 12 months to ensure there are no filter-related complications.
Table 1
Prior to the development of the VTE team, there were 243 IVCFs placed at our Prior to the development of the VTE team at Stony Brook, there were 243 IVCFs placed at our institution over a two-year period. Of these, only 9% were ultimately retrieved. After the VTE team was established, the total number of IVCF placement drastically decreased to less than 50 on average per year. Additionally, retrieval rate averaged 66% in the six years following the development of the VTE team (Table 1). The amount of patients lost to follow-up has also declined, with 2015 having only 2% of patients lost to follow-up (3/59 patients across three services). We have shown that a systematic strategy and a dedicated team for following patients will enhance filter retrieval even within a few months of establishing such a system. These results can be sustained several years after development of a specialized VTE team. This is mainly due to close communication with patients and their primary practitioners leading to decreased patients lost to follow-up, appropriate management of anticoagulation, and arrangement of timely retrieval. As such, it is critical the team must maintain efforts for continuous monitoring and follow-up, otherwise compliance can drop.
References
1. Guyatt GH, Akl EA, Crowther M, et al. Antithrombotic therapy and prevention of thrombosis, 9th ed: American College of Chest Physicians evidence-based clinical practice guidelines. Chest 2012;141(2_suppl):7S-47S.
2. Tao MJ, Montbriand JM, Eisenberg N, et al. Temporary inferior vena cava filter indication, retrieval rates, and follow-up management at a multicenter tertiary care institution. J Vasc Surg 2016;doi:10.1016/j.jvs.2016.02.034.
3. PREPIC Study Group. Eight-year follow-up of patients with permanent vena cava filters in the prevention of pulmonary embolism: the PREPIC (Prevention du Risque d’Embolie Pulmonaire par Interruption Cave) randomized study. Circulation 2005;112:416-422.
4. United States Food and Drug Administration. Removing retrievable inferior vena cava filters: initial communication, www.fda.gov/MedicalDevices/Safety/AlertsandNotices/ucm221676.htm (2010, accessed 6 June 2016).
5. O’Keeffe T, Thekkumel JJ, Friese S, et al. A policy of dedicated follow-up improves the rate of removal of retrievable inferior vena cava filters in trauma patients. Am Surg 2011;77:103-108.
6. Gasparis AP, Spentzouris G, Meisner RJ, et al. Improving retrieval rates of temporary inferior vena cava filters. J Vasc Surg 2011;54:34S-38S.
7. Minocha J, Idakoji I, Riaz A, et al. Improving inferior vana cava filter retrieval rates: impact of a dedicated inferior vena cava filter clinic. J Vasc Interv Radiol 2010;21:1847-1851.
Learn more about IVC filter retrievals
Practice, as well as guidance from experts, is crucial as you develop mastery over the art and science of IVC filter retrieval. Cook Medical is ready to partner with you. You can focus on specific topics and learn from premier interventionalists with our Vista Education and Training Program on Cook devices:
View a procedural video showing how to retrieve Günther Tulip® Vena Cava filters:
Caution: U.S. Federal law restricts this device to sale by or on the order of physician (or properly licensed practitioner).
Contraindications:
• Retrieval of the filter with significant amounts of trapped thrombosis (greater than 25% of the volume of the cone).
• Retrieval of the filter for patients with an on-going high risk for pulmonary embolism (PE).
Warnings: This product contains NATURAL RUBBER LATEX which may cause allergic reactions. The latex component is in the Side-Arm Adapter.
Dr. Antonios Gasparis is a paid consultant for Cook Medical.